Men Should Discuss Potential Sperm Damage Before Starting Certain Medications
The Changing View on Male Fertility
There is more focus on male fertility now than ever before.
I have written articles highlighting the panicked testosterone statements from RFK Jr., why gay intended dads should care about their sperm, and lifestyle changes to improve sperm health.
However, I have not yet covered the impact of medications on sperm health.
While it is known that certain classes of drugs like those used in chemotherapy are especially toxic for sperm and fertility, there is less known about the impact of more common medications.
In a recent study, real world data was analyzed across the United States and Europe that identified medications potentially causing male infertility or sperm abnormalities.
What Does the Study Say?
The study leveraged two of the largest and most comprehensive databases on medications and adverse events:
United States Food and Drug Administration Adverse Event Reporting System (FAERS)
European Medicines Agency EudraVigilance (EV) database
The authors analyzed over 20 years of data from each of these databases and identified 1,955 cases in FAERS and 1,384 cases in EV of medication-related male infertility and/or sperm damage.
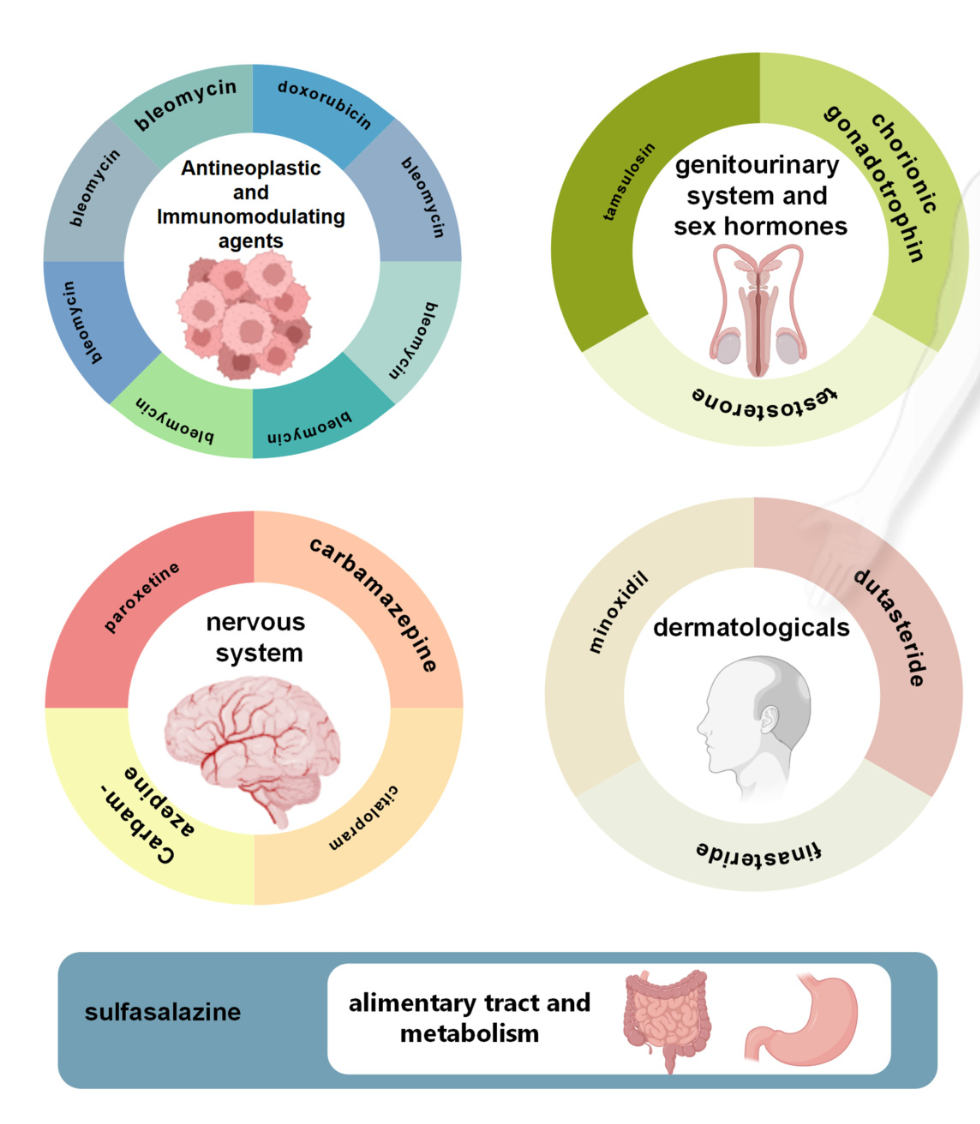
This figure from the paper shows the drug classes and specific generic drug names that were the biggest offenders:
The results showed that 45% of events (e.g. a diagnosis of sperm issues or infertility) occurred within 100 days from taking a medication. This demonstrates a stronger possible link between the medication’s effect and the sperm lifecycle of about 3 months. While this time from starting the medication to the diagnosis or ‘event’ was only available for about one fifth of the cases, it does suggest a stronger causal relationship.
Chemotherapy medications (antineoplastic and immunomodulating agents in the picture above) as well as hormonal treatments like testosterone (genitourinary system and sex hormones in the picture above) are not surprising categories to have shown up in these real world data. The implications of these medications on male fertility has been well described.
What I found most interesting about these data is the range of common medications that are associated with male infertility:
Medications for male pattern baldness (e.g. finasteride, dutasteride, minoxidil)
Medications for depression (e.g. SSRIs)
Medications for ADHD (e.g. SNRIs)
These medications are used by millions of men around the world, and I believe there is little to no counseling on the fertility impacts of these medications before they are initiated.
What are the Trends in Usage of Common Drugs that Affect Male Fertility?
I wanted to focus on 4 common drug classes and describe their usage trends and impacts on sperm.
Finasteride
It is estimated that over 2 million men use finasteride in the United States alone.
In the U.S., finasteride prescriptions in men over the age of 25 have increased 200% over the last 7 years.
Prolonged use of more than 18 months has been shown to significantly diminish semen parameters, with patients treated for more than 20 months potentially experiencing persistent impairment even after stopping the medication.
SSRIs (Selective serotonin reuptake inhibitors)
8.4% of US adult men are on anti-depressants with SSRIs being the most common.
SSRIs significantly reduce sperm morphology (shape), concentration, and motility (movement) while increasing DNA fragmentation.
SNRIs (Serotonin norepinephrine reuptake inhibitors)
The SRNI atomoxetine was used by over 700,000 patients in the US in 2023.
Atomoxetine is used to treat ADHD, with diagnoses on the rise. In the United Kingdom between 2000 and 2018, rates doubled in boys under 18 and increased 20-fold in men over 18.
Testosterone
In the U.S., testosterone usage has increased from about 7.3 million men in 2019 to over 11 million men in 2024, an increase of almost 50%.
Testosterone causes negative feedback on sex hormones, causing over 90% decline in the body’s own testosterone production and almost completely stops sperm creation.
Studies have shown that sperm concentration and hormonal recovery take an average of 8.5 months after discontinuing testosterone.
It’s important to distinguish that if a patient has diagnosed low testosterone then supplementation can actually help fertility. However, for men taking testosterone to get supraphysiologic levels and wellness benefits, this leads to the opposite effect on sperm creation and health.
While the study covers a number of other medications and their impacts on sperm health, I think these are most relevant for their common and increasing usage and lack of awareness on the male fertility impact.
Implications for Men Pursuing Family Building
So what should be done with this information?
The first step is education. Young men - even men who are years away or not sure if they want to have kids - should have discussions with their providers before starting any of these medications.
Fertility side effect education is done routinely when men are undergoing cancer treatment and offered fertility preservation such as sperm freezing. However, I have serious doubts if any twenty-something with thinning hair is thinking about or counseled on his sperm health when asking for Rogaine or Propecia. If a man uses these medications for over two years, there is a chance this could result in permanent sperm health issues.
The same goes for SSRIs, SNRIs, and testosterone. These can be essential medications, but patients should be counseled on their impacts and discuss alternatives or transitioning off these treatments safely around the time they are trying to have a child.
The lifecycle of sperm is about 3 months. Temporary medication changes under a physician’s supervision can be made if someone is considering starting a family or planning for IVF. Giving sperm the greatest possible chance to be healthy is crucial for successful family building.
It’s important for all men, even gay men who are considering IVF and surrogacy, to think about the current and future implications cosmetic and prescription medication can have on their fertility. Real world evidence like this study provides more evidence that classes of medications are more detrimental to sperm. This is empowering for providers and patients in order to help mitigate some of the increasing challenges around male fertility.